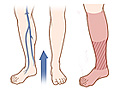
Venous Skin Ulcer
Condition Basics
What is a venous skin ulcer?
A skin ulcer is a type of wound that develops on the skin. A venous skin ulcer is a shallow wound that occurs when the leg veins don't return blood back toward the heart the way they should. This is called venous insufficiency.
These ulcers usually form on the sides of the lower leg, above the ankle and below the calf.
Venous skin ulcers are slow to heal and often come back if you don't take steps to prevent them.
A venous skin ulcer is also called a stasis leg ulcer.
What causes it?
Venous skin ulcers are caused by poor blood circulation from the legs, such as from venous insufficiency. Your veins have one-way valves that keep blood flowing toward the heart. In venous insufficiency, the valves are damaged, and blood backs up and pools in the vein. Fluid may leak out of the vein and into the surrounding tissue. This can lead to a breakdown of the tissue and an ulcer.
Veins that become blocked also may cause fluid to pool, leading to these ulcers.
Some things can increase your risk of venous skin ulcers. These include:
- Deep vein thrombosis, in which a blood clot (thrombus) forms in the deep veins of the legs.
- Obesity.
- Smoking.
- Lack of physical activity.
- Work that requires many hours of standing.
There are two other types of skin ulcers that can happen on the lower leg or feet. They are different from venous skin ulcers.
- Arterial skin ulcers are less common than venous skin ulcers. They happen when artery disease is present (sometimes in combination with venous disease). These ulcers tend to be extremely painful. They are usually on the toes and feet.
- Neuropathic skin ulcers are also known as diabetic neuropathic ulcers. They occur in people who have little or no sensation in their feet because of diabetic nerve damage.
What are the symptoms?
The first sign of a venous skin ulcer is skin that turns dark red or purple over the area where the blood is leaking out of the vein. The skin also may become thick, dry, and itchy.
Without treatment, an ulcer may form. The ulcer may be painful. You also may have swollen and achy legs.
If the wound becomes infected, the infection may cause an odor, and pus may drain from the wound. The area around the wound also may be more tender and red.
Call your doctor when you first notice the signs of a venous skin ulcer, because you may be able to prevent the ulcer from forming. If an ulcer has formed, get treatment right away, because new and smaller ulcers tend to heal faster than larger ones.
How is it diagnosed?
Your doctor will diagnose venous skin ulcers by asking questions about your health and looking at your legs. Your doctor may also use duplex Doppler ultrasound to find out what is causing the ulcer. This test shows how well blood is moving through the lower leg.
Your doctor may use other tests to check for problems related to venous skin ulcers or to recheck the ulcer if it does not heal within a few weeks after the start of treatment.
How is a venous skin ulcer treated?
The first step involves improving blood circulation. To do this, you can:
- Lift your legs above the level of your heart as often as possible. For example, lie down and then prop up your legs with pillows.
- Wear compression stockings or bandages. These help prevent blood from pooling in your legs.
- Walk daily. Walking helps your blood circulation.
To help your ulcer heal, your doctor may also remove dead tissue from the wound (debridement).
After your ulcer has healed, continue to wear compression stockings. Take them off only when you bathe and sleep. Compression therapy helps your blood circulate and helps prevent other ulcers from forming.
If your ulcer doesn't heal within a few months, your doctor may advise other treatment, such as:
- Medicine to speed healing or get rid of an infection (antibiotics).
- Skin grafting, which may be needed for deep or hard-to-heal ulcers.
- Vein surgery, which may keep ulcers from coming back.
What are some different types of compression therapy?
Compression therapy is the main treatment for venous skin ulcers. If you have a venous skin ulcer, your doctor may first want to reduce the buildup of fluid in your lower leg. After your lower-leg swelling has been reduced, compression is used to create more constant pressure on both the flexing and resting leg muscles. There are several types of medical devices for compression therapy. Your doctor will recommend the type that will work best for you. If you have an open wound, it will be covered with a dressing before the compression device is applied.
- Unna boot.
-
This is a stiff bandage made with gauze and zinc oxide paste wrapped around the lower leg. This type of bandage improves blood flow by putting greater pressure on leg muscles when they are flexing and less pressure on the leg during rest. It is used to reduce a large amount of swelling in your lower legs. An Unna boot can be left on for 7 to 10 days.
- Long-stretch bandage or short-stretch bandage.
-
These are flexible bandages that are wrapped tightly around the lower leg to reduce swelling and improve blood flow. The bandages are used to help heal a venous ulcer. The ulcer is covered with a dressing before the bandage is put on. The bandage is put on the leg by a health professional. Caregivers can be trained to apply them too.
- Active compression pump.
-
This pump goes around your lower leg. It has air bags that inflate and deflate periodically to force blood to flow out of your lower leg toward your heart. The pump can be used to help heal a venous ulcer that has not been helped by other types of treatment. The pump is used for several hours each day. It is used along with compression stockings.
- Compression stockings.
-
Specially fitted compression stockings are designed to help prevent fluid from pooling in the legs. You should wear these stockings every day from the time you wake up until you go to bed. Remove them only for bathing and sleeping. They can help venous skin ulcers heal and help prevent them from coming back.
Related Information
Credits
Current as of: December 4, 2024
Author: Ignite Healthwise, LLC Staff
Clinical Review Board
All Ignite Healthwise, LLC education is reviewed by a team that includes physicians, nurses, advanced practitioners, registered dieticians, and other healthcare professionals.
Current as of: December 4, 2024
Author: Ignite Healthwise, LLC Staff
Clinical Review Board
All Ignite Healthwise, LLC education is reviewed by a team that includes physicians, nurses, advanced practitioners, registered dieticians, and other healthcare professionals.